|

|

|
Toxical effect of blood in the subarachnoïdia
About blood in subarachnoid space, Arachnoïditis and Meningeal cysts.
(Charles Burton Burton reports)
The subarachnoid space represents the "salum sanctorum" of the human body. It abhors all foreign body substances. Even the presence of injected air is considered to be a "foreign body." Blood is definitely considered a foreign body (particularly the breakdown products of blood ). Repeat exposure to foreign body substances in the subarachnoid space can initiate auto-immune amnestic reactions which may potentiate and magnify the ongoing inflammatory process.
Few clinicians appreciate that significant pathologic change can occur unaccompanied by clinical symptoms because of the body's remarkable ability to adjust to, and compensate for, slowly occurring insult . This is particularly true of nervous system which does not respond well to acute change or acute insult (i.e. sudden trauma, acute intracranial hemorrhage or acute rupture of an aneurysm). The ability of the body to compensate is an important reason why most individual afflicted with adhesive arachnoiditis have few in the way of clinical symptoms. This state is, however, a tenuous one, which can change dramatically with only minimal additional insult.
Because of the factors noted above the presentation and the nature of FAS, may, not unexpectedly, vary in individual cases. This is due, in large part, to each individual's unique immnunologic response to the progression of acute and chronic inflammation.
We live in a medical era still characterized by lumbar puncture routinely utilized for the following purposes:
Initiation of spinal anesthesia.
Diagnostic taps to obtain spinal fluid samples, i.e. to rule out meningitis.
We also live in a medical era where frequent (inadvertent) lumbar punctures are performed by ill-advised blind-technique in cases of attempted epidural steroid administration or epidural anesthesia..
It is not unusual for patients to experience, as a complication of spinal tap, continued leakage of cerebro-spinal fluid producing postural headache, lightheadedness and inability to function due to these complaints. The commonly employed treatment for this is a "blood patch." Blood drawn from a vein is purposely injected into the supposed epidural space as a means of "patching" the leaking fluid.
Appropriate blood patches routinely introduce some blood into the subarachnoid space and inappropriate ones may introduce as much as 10-12cc of blood directly into the subarachnoid space. How much blood, introduced how often, is necessary to create adhesive arachnoiditis? This question has not yet been answered. We only know at this point in time, that blood, and its breakdown products, can serve to create adhesive arachnoiditis and the introduction of any foreign body substance (for any purpose) into the subarachnoid space is not a wonderful idea.
Not to forget to mention that arachnoïd cysts, meningeal cysts are very frequently induced by a dormant Arachnoïditis and that only that area of the spine, where the cysts are can be the cause for neuropatic pain and a limitation of functions syndrome.
more about the arterioveinous "track"
The arterioveinous "track" is now more and more told about by researchers (thanks to all new devices) and the toxical effect of any bleeding inside a nerve or close to a nerve as an major event leading to meningeal problems, pain and symptoms, meningeal syndrome.
This is very important as new means confirm findings of the past, explain why several patients, with adapted treatment are now back to quite no symptoms, without surgery, and that so many are worse with a surgery.
Modern understanding of the non-infectious neuropathologic entity "adhesive arachnoiditis" began in 1926 with the publication "La Myélite nécrotique subaiguë (Myélite central angiohypertrophique évolution progressive). Paraplégie amyotrophique lentement ascendan d'abord spasmodique, puis flasque" by authors C. Foix and T. Alajounanine in the French Revue Neurologique (Paris), 2: 1-42). What these authors described were cases which, in all probability, represented primary spinal cord arteriovenous malformations ("A-V Mals") producing recurrent subarachnoid hemorrhage. The blood, and breakdown products, acting as a foreign body substance in the subarachnoid space produced local adhesive arachnoiditis. The progression of this inflammation acted to not only infarct the spinal cord producing myelomalacia (and sometimes also creating cystic degeneration) but also the clinical symptoms of transverse myelitis and associated progressive loss of function in the lower body (i.e. paraplegia).
This means that most individuals afflicted with this neuropathologic entity may be completely asymptomatic despite living with a "sword" hanging over their heads. This balance is, however, often a tenuous one and can be upset by something as simple as a routine epidural anesthetic administered during childbirth.
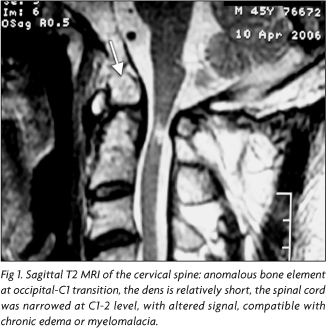
|
|